Shockwave Therapy vs Injections: Which Is Better for Pain Relief?

When pain does not go away on its own, most people start looking for options that offer more than temporary relief. Stretching and medication may help at first, but once pain becomes persistent, the conversation usually turns to more targeted treatments.
Two of the most common options discussed in pain clinics today are shockwave therapy and injections. Both aim to reduce pain and improve function, but they work in very different ways. One stimulates the body’s natural healing response. The other delivers medication directly to a problem area.
If you are deciding between these approaches, the right answer depends on how your pain started, how long it has been present, and what is driving it beneath the surface. Understanding the differences can help you make a more informed decision and avoid treatments that do not match your condition.
Why Pain Relief Is Not One Size Fits All
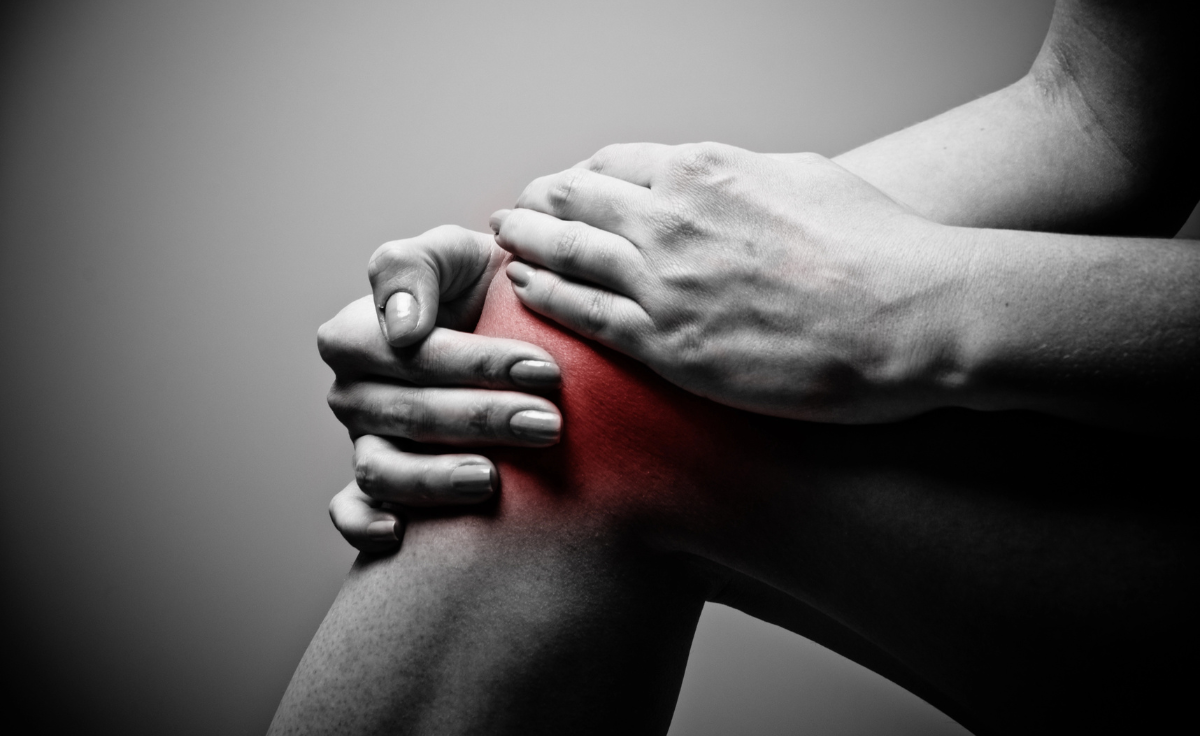
Pain is not a single condition. It can come from irritated tendons, strained muscles, inflamed joints, compressed nerves, or altered movement patterns. Two people with pain in the same location may need entirely different treatments.
This is why choosing between shockwave therapy and injections should never be based on convenience alone. Each approach targets a different mechanism of pain. When used correctly, both can be effective. When mismatched ,results are often disappointing.
Pain specialists focus on identifying what is actually generating pain before recommending either option.
Also Read: How to Choose the Right Pain Management Specialist in Los Angeles
What Shockwave Therapy Actually Does
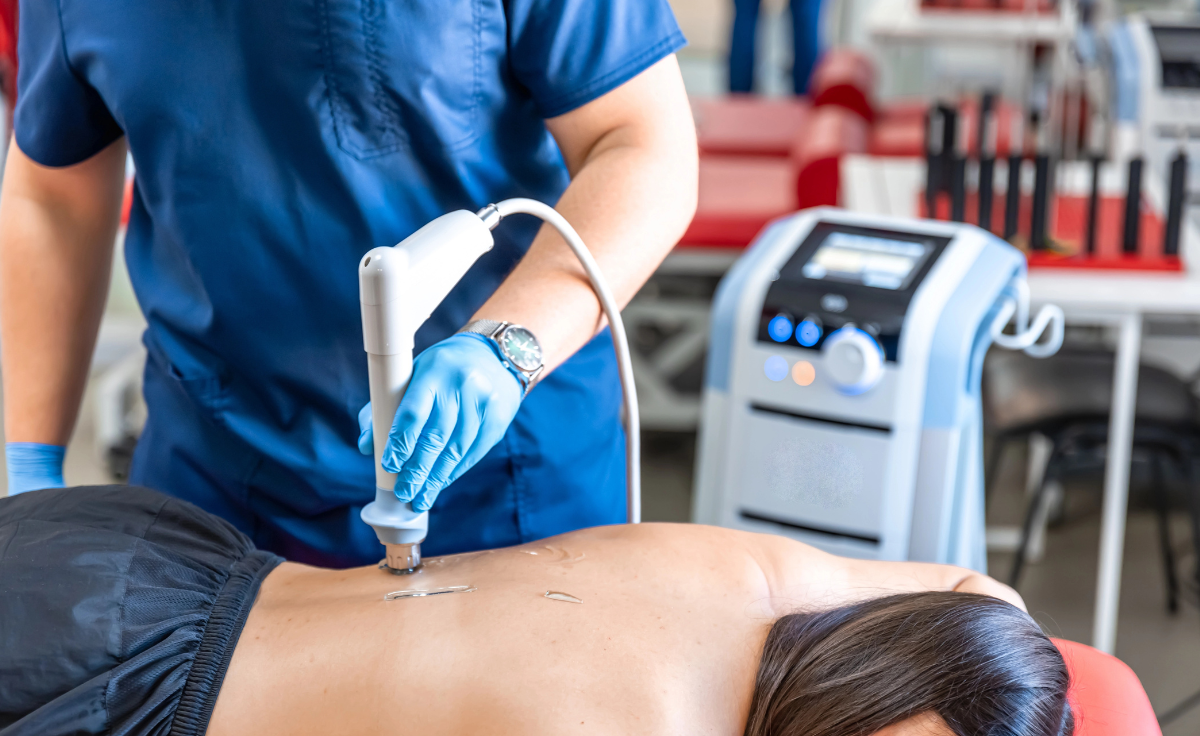
Shockwave therapy, formally known as extra corporeal shockwave therapy (ESWT), uses high-energy acoustic waves. These are mechanical pressure pulses, not electrical shocks. The goal is not to numb pain. The goal is to stimulate biological change in tissue that has stopped healing on its own.
A handheld device delivers the waves through the skin into targeted structures. Where the energy reaches damaged tissue, it creates controlled microtrauma. That microtrauma is intentional. It signals the body that healing needs to begin again.
When shockwave energy reaches injured tissue, it can increase blood flow, activate growth factors, stimulate collagen production, and support tissue remodeling over time. This is why shockwave therapy is often used for chronic tendon and fascia conditions that tend to stall, especially in areas with limited circulation.
Shockwave therapy is commonly used for conditions like plantar fasciitis, Achilles tendinopathy, tennis or golfer’s elbow, rotator cuff degeneration, and other chronic soft tissue injuries that have not improved with rest alone.
The goal is not to mask symptoms. The goal is to restart a healing process that stalled.
What Shockwave Therapy Feels Like
During treatment, you feel rhythmic pulses directed at the painful area. Most patients describe it as deep tapping, heavy thumping, or a strong pressure sensation. It can feel more intense over bony areas or highly sensitive points, but sessions are brief, and the intensity can be adjusted in real time.
There is no anesthesia, no injection, and no downtime afterward. You can return to daily activities the same day. Patients are often advised to avoid high-impact activity for a short period, not because the tissue is fragile, but because the body is beginning a repair cycle and needs space to initiate it.
Improvement typically occurs gradually. This is not a numbing treatment. Tissue remodeling unfolds over weeks, and many patients notice their biggest improvement several weeks after treatment is complete.
What Injections Are Designed to Do
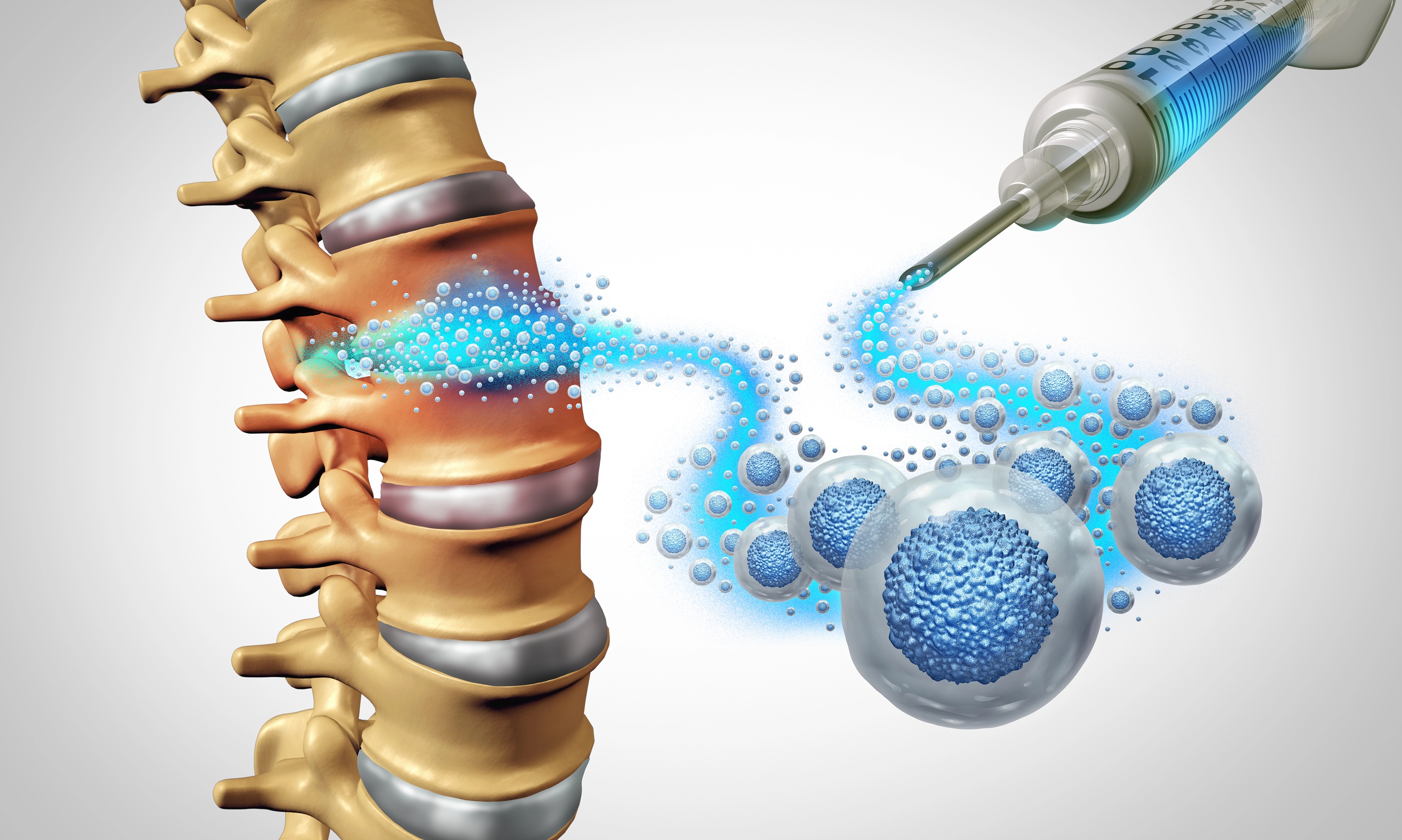
Injections work by delivering medication directly to a specific structure. The most common types used in pain management are corticosteroid injections and local anesthetic injections.
Steroid injections reduce inflammation quickly. They are often used for joint pain, bursitis, and nerve irritation. Local anesthetics provide temporary pain relief and are sometimes used diagnostically.
Unlike shockwave therapy, anti-inflammatory injections such as corticosteroids are designed primarily for symptom control. They can be helpful when inflammation is driving pain, or when discomfort is so severe that it prevents movement and rehabilitation.
What Injections Feel Like and What to Expect
Injections involve a needle placed into or near the painful structure. Sensation varies based on the area and individual sensitivity. Some injections provide rapid relief, while others take days to become noticeable.
Relief from steroid injections may last weeks or months, but it is often temporary. In some cases, repeated steroid injections can contribute to tissue weakening over time, which is why they are typically limited and used strategically rather than indefinitely.
Depending on the type of injection and location, patients may be advised to modify their activity for a short period afterward.
The Key Difference Between These Treatments
Shockwave therapy is designed to stimulate the body’s own healing response and aims to change the tissue environment over time. It works by stimulating a biological healing response, especially in tendons, fascia, and other structures where healing has stalled.
Many anti-inflammatory injections aim to quiet inflammation or reduce pain signals quickly. They can be extremely useful for flares and acute inflammation, but they do not always change the underlying tissue quality that allows pain to persist.
Neither approach is inherently better. The effectiveness depends on matching the treatment to the condition.
When Shockwave Therapy Tends to Be the Better Option
Shockwave therapy is often the stronger choice when pain is chronic and structural, especially when symptoms suggest stalled healing.
Common patterns include pain lasting longer than three months, pain that improves briefly with rest but returns with activity, localized tenderness over a tendon or fascia, and stiffness that loosens with movement but returns later.
If imaging or examination suggests tendon degeneration, thickened fascia, or calcification rather than acute inflammation, shockwave therapy often aligns better with the biology of the problem. It is also a good option for patients who want to avoid medication, repeated steroid injections, or more invasive procedures.
Patients who respond well often notice gradual improvement in pain, function, and confidence in movement rather than immediate but short-lived relief.
When Medicated Injections May Be the Better Choice
Medicated injections can be appropriate when inflammation plays a dominant role. Acute joint flare-ups, severe bursitis, or nerve irritation may respond quickly to targeted medication.
Injections may also help when pain is so limiting that it prevents participation in physical therapy or rehabilitation .In these cases, reducing pain or inflammation can create a short window where movement becomes possible again.
Pain specialists use injections strategically. The goal is to support recovery, not to rely on injections indefinitely.
Why Some Patients Get Poor Results From Either Treatment
Poor outcomes usually come from misdiagnosis rather than treatment failure. This is why evaluation matters more than the treatment itself. Pain specialists assess movement patterns, posture, muscle balance, joint mechanics, and activity demands before recommending either option.
Can Shockwave Therapy and Injections Be Used Together?
In some cases, yes.
A patient may benefit from an injection to calm a severe flare or reduce acute inflammation, followed by shockwave therapy to support longer-term tissue healing. In other cases, shockwave therapy may be used first to promote regenerative change, with injections reserved only if symptoms suggest a different mechanism.
The key is coordination. Using both treatments without a clear plan often leads to frustration. Timing and diagnosis matter.
Safety Considerations You Should Know
Shockwave therapy is non-invasive and carries minimal risk when performed appropriately. Temporary soreness, redness, or mild bruising can occur, but most side effects are short-lived.
Injections carry small but meaningful risks, including infection, tissue irritation, and systemic effects depending on the medication used. With steroid injections in particular, risks can increase with frequency, which is why providers typically limit repeated use.
Pain specialists weigh these risks carefully when building a plan.
Why Early Decision-Making Matters
The longer the pain persists, the more complicated the treatment can become. Chronic pain often leads to compensation patterns, reduced activity, muscle imbalance, and nervous system sensitization.
Early evaluation makes it easier to match treatment to the underlying cause while options are still conservative and recovery is more straightforward.
Waiting often limits options.
How Pain Specialists Decide What Is Right for You
At The Pain Free Institute, treatment decisions are never based on a single symptom or imaging finding.
Your evaluation includes a detailed history, physical examination, and assessment of how pain affects your movement and daily life. If needed, imaging such as ultrasound or MRI may help confirm whether tissue is inflamed, degenerated, or calcified.
Shockwave therapy, injections, or a combination may be recommended based on what is driving your pain, not what is most commonly offered. This approach improves outcomes and helps avoid unnecessary procedures.
Also Read: Shockwave Therapy Myths vs. Facts: What Patients Should Know Before Treatment
Pain Relief Should Support Function, Not Replace It
Effective pain treatment does more than reduce discomfort. It restores movement, confidence, and participation in daily life.
Whether shockwave therapy or injections are appropriate, your care plan should move you toward long-term improvement rather than short-term symptom control alone.
Making the Right Choice Starts With the Right Evaluation
If you are weighing shockwave therapy against injections, the most important step is understanding your diagnosis.
The specialists at The Pain Free Institute focus on identifying the true source of pain and matching treatment accordingly. Care is personalized, evidence-based, and designed to support lasting recovery.
Schedule a consultation today to learn which option fits your condition and start moving toward real pain relief.

.svg)



.svg)











.webp)

.png)

.png)
.png)