Are PRP Injections Safe for Long-Term Joint Health?

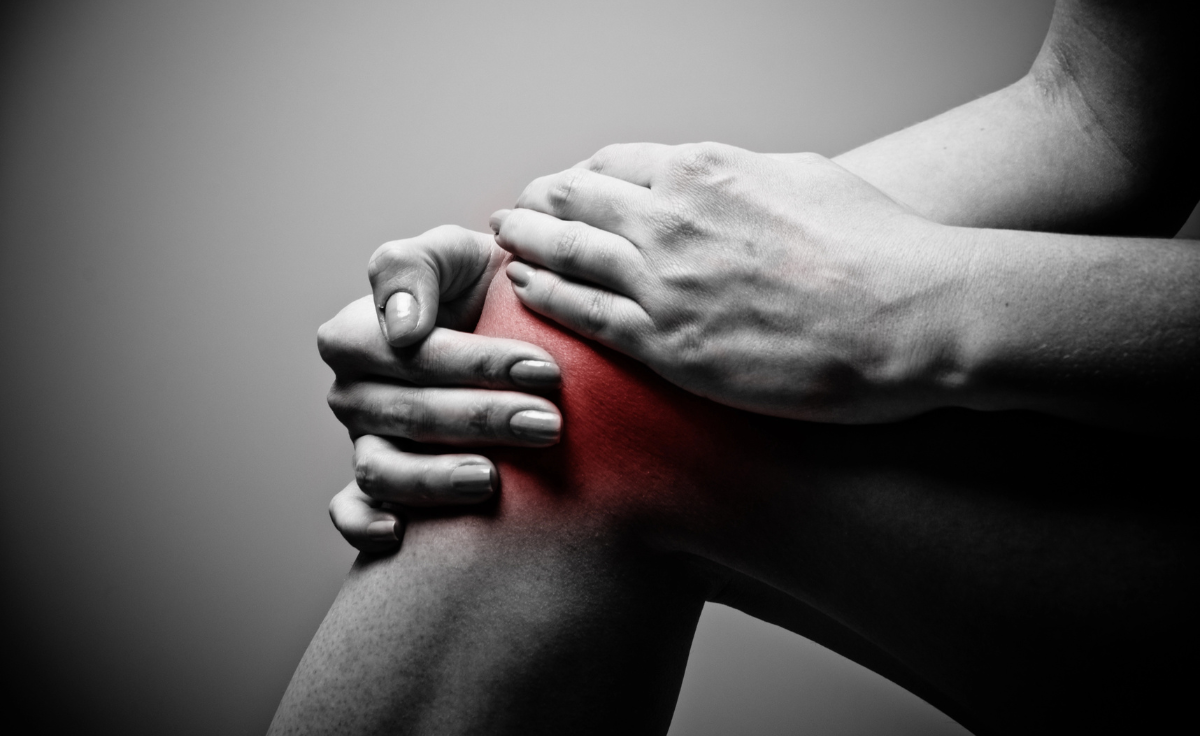
Chronic joint discomfort can feel like a heavy weight on your daily life. It might be a knee that clicks with every step or a shoulder that protests when you reach for a shelf; finding a way to move without pain is a top priority for many. As more people look for ways to stay active without resorting to surgery, PRP injections have become a frequent topic of conversation.
At The Pain Free Institute, we see patients every day who want to know whether platelet-rich plasma is just a quick fix or offers lasting relief. More importantly, they want to know: Are PRP injections safe for long-term joint health?
Why Patients Ask About Long-Term Safety
Over the last decade, PRP therapy has moved from the side lines of professional sports medicine into main stream clinics. This rise in popularity stems from a shift in how we view healing. Instead of just masking symptoms, patients are looking for ways to support the body’s natural repair processes.
When people hear about any injectable treatment, they naturally worry about side effects. “Will this damage my joints over time?” or “Can I get too many of these?” are valid questions. Because many patients are used to the limitations of traditional medicine, they approach regenerative medicine with a cautious eye toward the future.
Most traditional treatments for joint pain rely on synthetic chemicals. Over-the-counter pills can be hard on the stomach and kidneys when used for years. Steroid shots,while helpful for immediate swelling, have a reputation for weakening tissues if used too often. PRP injections stand apart because they do not rely on outside chemicals to do the work.
What PRP Actually Is
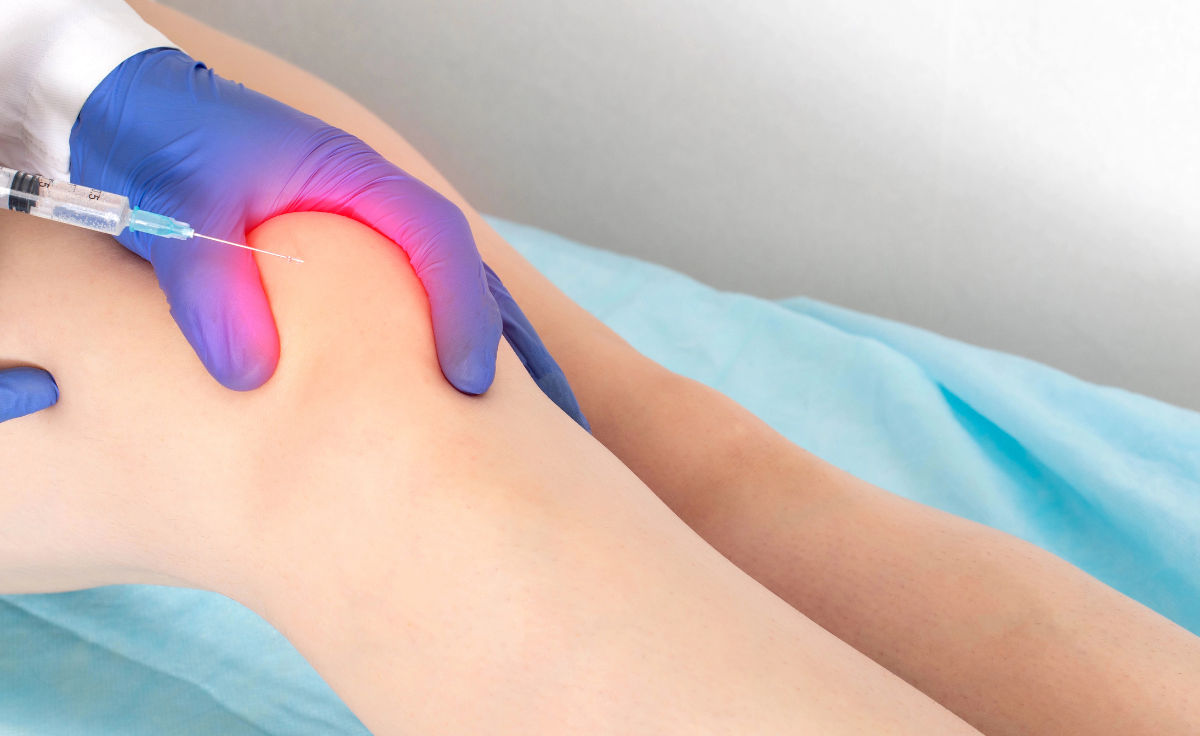
The process starts with a simple blood draw from your arm, much like a standard lab test. That blood is placed into a centrifuge, a machine that spins rapidly. This spinning separates the blood into different layers. We isolate the plasma that contains a high concentration of platelets.
Platelets are best known for helping blood clot, but they are also tiny power houses of growth factors. These proteins act as messengers. When a high concentration of these messengers is introduced to a site of wear and tear, they signal the body to begin repair work.
Because the substance comes from your own body, it is labeled a biologic. This means there is no risk of an allergic reaction or your body rejecting the treatment. You are simply taking the healing tools you already possess and placing them exactly where they are needed most.
How PRP Works Inside a Joint
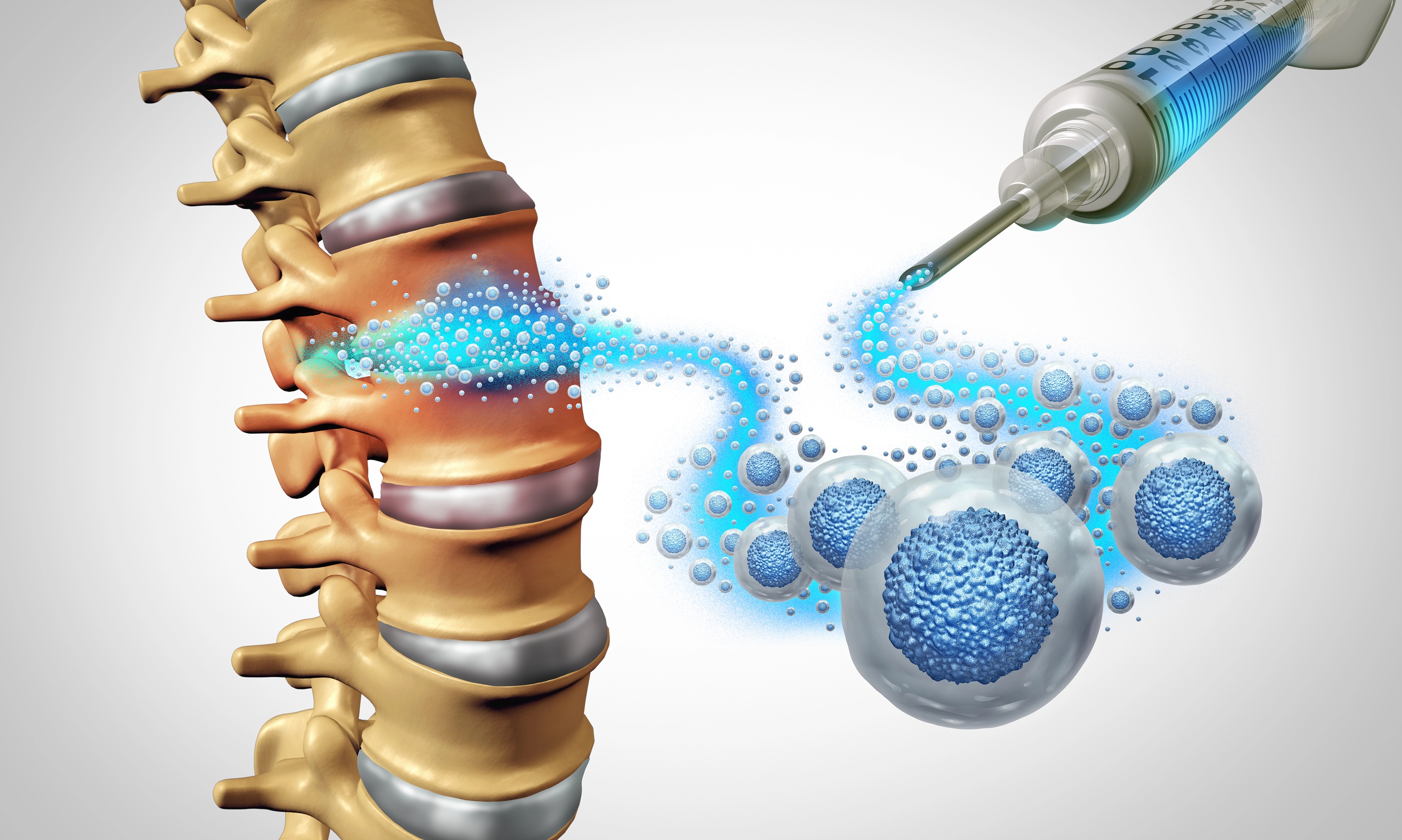
Many joint issues involve a cycle of chronic inflammation that breaks down tissue. While some treatments aim to just shut down that inflammation, PRP therapy aims to shift the environment inside the joint. It moves the area from a state of constant breakdown to a state of potential repair.
Once injected, the platelets release their growth factors over the first several days. These factors help attract repair cells to the area. For joint health, this means supporting the cells that maintain cartilage and the joint lining.
In the days following the procedure, it is normal to feel some soreness. This is actually a sign that the body is responding. Unlike a numbing agent that works in minutes, PRP takes time. The real work happens beneath the surface over the course of several weeks.
PRP vs. Cortisone: A Safety Comparison
Today’s pain management options extend beyond a one-size-fits-all approach. While PRP and cortisone are two well-known treatments, they reflect different philosophies of care. Understanding whether a treatment is designed for short-term relief or longer-term tissue support can help patients choose an approach that aligns with their needs and lifestyle.
Cortisone is a powerful anti-inflammatory. It is excellent for reducing swelling and calming acute flare-ups. However, it does not repair damaged tissue. In contrast, PRP joint therapy at The Pain Free Institute focuses on supporting the joint's structure over time.
Research has shown that repeated corticosteroid injections can contribute to thinning of joint cartilage and weakening of tissues in some patients, while PRP helps preserve existing cartilage.
Because of these risks, physicians often limit how frequently steroid injections can be given. PRP does not carry the same concerns about long-term tissue damage, making it amore suitable option for patients thinking beyond short-term relief.
Also Read: PRP vs. Cortisone: Which Injection Works Better for Long-Term Pain Relief?
Is PRP Safe Over Time?
Data from years of clinical use suggest that PRP has a strong safety profile. Because it is autologous (derived from your own body), the long-term risks of PRP therapy for joints are minimal compared to synthetic medications.
As with any injection, there is a very small risk of infection at the injection site. However, because PRP uses your own blood, there is no risk of allergic reaction or toxicity from foreign substances.
Over time, the injected plasma is naturally absorbed by the body. There is no buildup of material left behind, only the biological signals that help support healthier joint function.
How Often Can PRP Be Used?
Most patients see meaningful improvement from a single injection or a short series of two to three treatments, typically spaced several weeks apart.
Some patients choose to receive a maintenance or booster injection every year or every eighteen months, depending on activity level and joint condition.
Many notice gradual improvements such as reduced stiffness, improved range of motion, and less reliance on daily pain medications, signs that the joint environment is becoming more stable.
Who Is a Good Candidate for PRP
PRP works best when there is still viable tissue within the joint. Early to moderate joint degeneration often responds better than end-stage arthritis.
Patients who want to remain active, running, golfing, or simply moving comfortably often choose PRP as a way to delay or avoid surgery.
For younger patients or those not ready for joint replacement, PRP can help preserve function and manage symptoms over the long term.
When PRP May Not Be Enough
If cartilage loss is severe or the joint is completely bone-on-bone, PRP may have limited benefit.
Mechanical issues such as major ligament tears or structural blockages cannot be corrected with injections alone.
At The Pain Free Institute, we are transparent about limitations. When PRP is unlikely to provide meaningful benefit, we help guide patients toward appropriate next steps, including surgical consultation when necessary.
What a Proper PRP Program Includes
We don’t guess. Imaging, such as X-rays or MRI, helps us understand the condition of the joint and determine whether PRP is appropriate.
When needed, we may use ultrasound guidance to ensure accurate placement. For larger joints like the knee, Dr. Farnad is able to deliver PRP injections precisely without ultrasound, based on anatomy and experience. Ultrasound is used selectively, not automatically, depending on the joint and clinical situation.
PRP is rarely a stand alone solution. We may pair injections with targeted movement plans or physical therapy to support long-term joint health and function.
Choosing a Path for Joint Pain Treatment
Choosing a path for joint pain treatment is a meaningful decision. When considering the long-term safety of PRP injections, the evidence supports a therapy that works with the body’s natural biology rather than against it.
At The Pain Free Institute, PRP joint therapy is used thoughtfully, with precision, and only when appropriate. If you are tired of temporary fixes and want to explore regenerative options, our team is here to help you determine whether PRP is the right step toward staying active and comfortable for years to come.

.svg)



.svg)











.webp)

.png)

.png)
.png)