PRP vs. Cortisone: Which Injection Works Better for Long-Term Pain Relief?

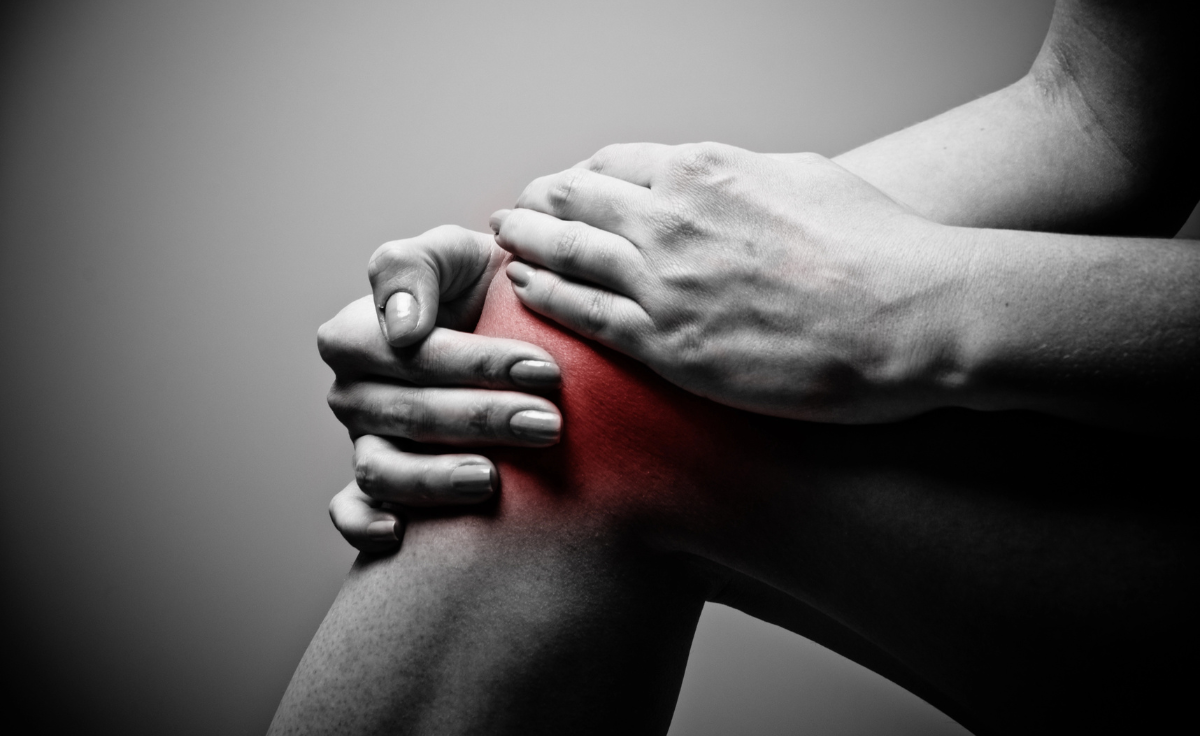
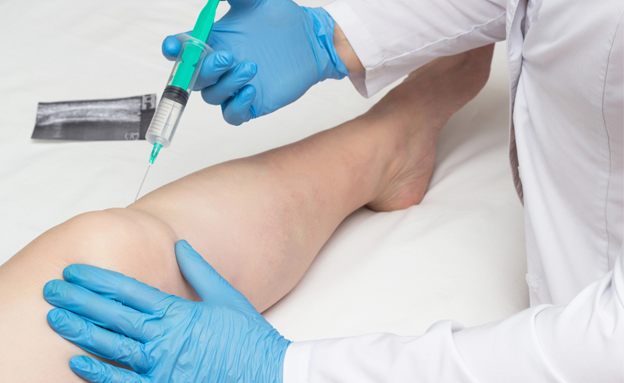
Many people turn to injection therapy for treatment of chronic joint, tendon, or soft-tissue pain, especially when physical therapy or oral medications are not enough. These treatments deliver relief exactly where it is needed, helping you return to your daily activities.
However, not all injections are built the same. Today’s pain management options extend beyond a one-size-fits-all approach. While PRP and cortisone are two well-known treatments, they reflect different philosophies of care. Understanding whether a treatment is designed for short-term relief or longer-term tissue support can help patients choose an approach that aligns with their needs and lifestyle.
What Is Cortisone?
Cortisone is a powerful anti-inflammatory medication. It is a synthetic version of cortisol, a hormone your body produces naturally to manage stress and inflammation. When injected into a painful joint or tendon, it works by calming the immune response in that specific area.
Conditions Treated with Cortisone
Doctors frequently use cortisone for:
● Osteoarthritis flare-ups in the knee or hip
● Sudden, sharp inflammatory episodes
Why Patients Choose Cortisone
Cortisone is popular because it works fast. If you have a wedding coming up or a vacation where you need to walk, cortisone can provide that window of comfort. Most patients feel a significant drop in pain within 48 to 72 hours. It is designed to quiet the fire of inflammation so you can move again.
What Is PRP (Platelet-Rich Plasma)?
PRP takes a different approach. Instead of using a synthetic drug, it uses your own biology. To create PRP, a small amount of your blood is drawn and then centrifuged. This machine spins the blood at high speeds to separate the platelets from other blood components.
How PRP Supports Healing
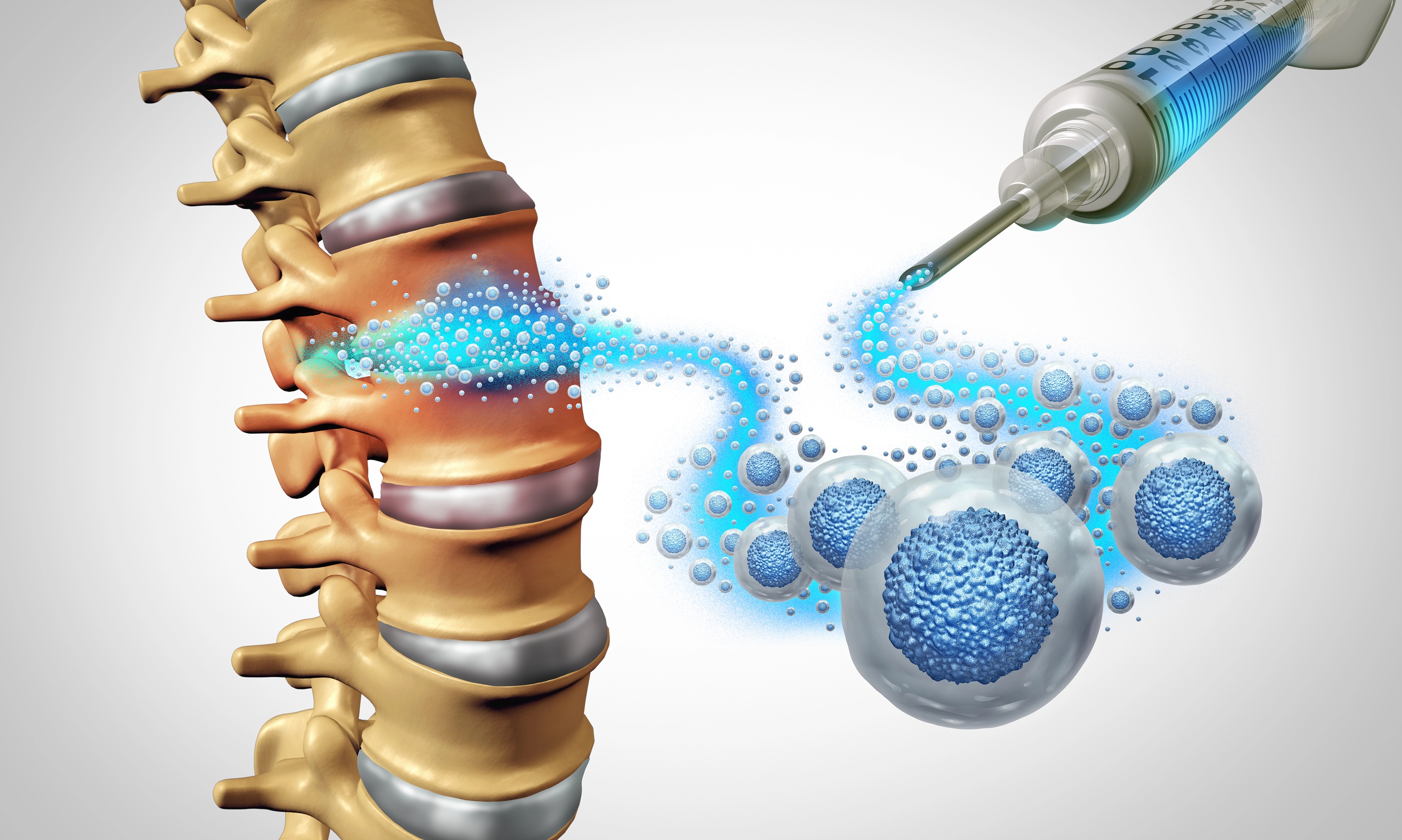
Platelets are the components in your blood responsible for clotting and repair. They contain growth factors that signal the body to fix damaged tissue. By concentrating these platelets and injecting them into an injured site, the treatment aims to jumpstart the body’s natural repair mechanisms.
Also Read: Regenerative Medicine & Alternative Therapies
Conditions Commonly Treated with PRP
● Chronic Tendon Injuries: This includes tennis elbow, golfer’s elbow, and Achilles tendonitis. These areas often have poor blood supply, making it hard for the body to heal them on its own.
● Ligament Sprains: Chronic instability in the ankle or knee, such as partial ACL or MCL tears, may benefit from the growth factors in PRP.
● Rotator Cuff Tears: Small or partial tears in the shoulder that cause weakness and pain during overhead movement.
● Plantar Fasciitis: Long-term heel pain that has not responded to stretching or orthotics.
● Early-Stage Osteoarthritis: PRP is increasingly used for knee and hip arthritis to help manage pain by improving the internal environment of the joint.
Unlike treatments that simply mask a symptom, PRP is regenerative. It doesn’t suppress pain signals; it attempts to improve the tissue environment. Instead of suppressing the immune system, it directs the immune system to focus its energy on a specific area of damage.
How Cortisone and PRP Work Differently
Symptom Management vs. Structural Healing
Cortisone is a tool for symptom management. It addresses pain and swelling resulting from injury or degenerative conditions. When the medication enters the joint, it binds to receptors that tell the body to stop producing inflammatory chemicals. This is excellent for comfort, but it does nothing to rebuild a thinning tendon or a worn-out cartilage layer.
PRP, by contrast, targets structural healing. It delivers a high concentration of growth factors to the site of injury. These growth factors trigger the body’s repair cells to fix small tears or strengthen weak connective tissue. While cortisone masks the problem, PRP tries to solve it.
Short-Term Relief vs. Long-Term Change
Cortisone provides short-term relief. It is a bridge to help a patient get through a painful period, but it is rarely a final solution. Because it does not fix the structure, the pain may return once the medication is processed by the body.
PRP is about long-term change. Because the goal is to alter tissue integrity, the improvements achieved during a PRP cycle are intended to persist. The change happens at a cellular level, aiming to create a healthier, more resilient joint that can withstand activity without needing constant chemical intervention.
Speed of Relief
If you are looking for an overnight fix, PRP might be disappointing. Because PRP relies on biological growth, results take time. Patients often feel increased soreness for a few days after a PRP injection, and the real benefits may not appear for four to six weeks.
In contrast, cortisone provides that quick win. Within a few days, the swelling subsides, and the sharp pain often resolves. However, this speed comes with a trade-off. The relief from cortisone is often temporary, whereas the improvements from PRP tend to build over several months as the tissue matures.
Duration of Results
When we discuss long-term relief, we must consider the timeline of the treatment’s effect.
● Cortisone Timeline: Relief typically lasts anywhere from a few weeks to a few months. Once the medication wears off, the pain often returns because the original problem, the worn cartilage or the torn tendon, is still there.
● PRP Timeline: Because PRP aims to repair tissue, the results can last a year or longer. Many patients find that once the healing process takes hold, they don’t need to return for frequent top-off injections.
Impact on Joint and Tissue Health
This is perhaps the most important distinction for anyone thinking about their health five or ten years down the road.
Scientific studies have shown that repeated cortisone injections can actually be harmful. High doses of steroids over time can weaken tendons and lead to the breakdown of joint cartilage. This creates a diminishing returns effect where each subsequent injection lasts for a shorter period and causes more wear and tear.
PRP, on the other hand, is favored for degenerative conditions because it is tissue-neutral or tissue-positive. It does not degrade the joint. In fact, it is often used specifically to slow down the progression of joint degeneration in active individuals.
Conditions Where Each May Be Appropriate
Cortisone makes sense when the pain is so severe that you cannot sleep or perform basic physical therapy. It can quiet the joint so you can start are habilitation program. PRP is often the better choice for those who want to avoid surgery or who have chronic injuries that refuse to heal.
Safety and Side Effects
Cortisone Risks
The side effects of cortisone include cortisone flare, temporary pain increase, skin thinning at the injection site, and potential spikes in blood sugar, which is a concern for people with diabetes. Long-term use can lead to bone thinning or weakened ligaments.
PRP Safety
Because PRP uses your own blood, the risk of an allergic reaction or rejection is virtually zero. The main side effect is temporary localized soreness or swelling as the body begins the repair process. It is a very clean, drug-free profile that appeals to those wary of synthetic chemicals.
Also Read: When Pain Becomes Chronic: Why Early Intervention Matters
Cost and Coverage Considerations
One of the biggest hurdles for patients is the financial aspect.
● Cortisone: Since it has been a standard of care for decades, it is almost always covered by insurance. The out-of-pocket cost is usually just a co-pay.
● PRP: Despite growing evidence of its success, many insurance companies still label PRP as experimental and do not cover it. This means PRP is usually a self-pay treatment.
While PRP has a higher upfront cost, many patients weigh this against the cost of repeated cortisone shots, lost time at work, and the eventual need for more invasive surgeries if the tissue continues to degrade.
Choosing the Right Option for Your Goals
Choosing between these two isn’t about finding a winner, but about matching the treatment to your life.
If you are an athlete with a chronic tear who wants to keep playing for years, PRP offers a biological advantage. If you are an older adult with a sudden, painful gout or bursitis attack that prevents you from walking, cortisone provides the relief needed to get back on your feet.
Your activity level, age, and the severity of your condition all playa role. A personalized plan should look at whether you simply need to stop the pain today or if you want to change the health of the joint for tomorrow.
Conclusion
Cortisone and PRP serve different purposes in the management of pain and injury. One acts as a powerful brake on inflammation, while the other acts as a fuel for natural repair. Neither is the right choice for every person in every situation.
Long-term relief depends on your goals, your specific diagnosis, and the timing of your symptoms. Cortisone calms inflammation in the short term, while PRP supports the repair of damaged tissue for the future.

.svg)



.svg)











.webp)

.png)

.png)
.png)